Developments in Technology
What a distance we have come from that glass syringe and a single type of insulin.
When I was diagnosed with type 1 diabetes in 1974, I was given a glass reusable insulin syringe, which I kept in a tray of methylated spirits, and a bottle of urine test strips, which changed colour if your urine glucose level was above 10 mmol/l, the level at which the kidneys start to shift glucose from your blood into the urine.
The injection devices moved on. Initially to plastic single-use disposable syringes, then to insulin pens. Now, the NovoPen Echo pen is calibrated in half units and will remind you of the number of units last injected and how many hours ago.
I use Humalog insulin with a Humapen, and I have attached a Timesulin timer which I bought, to record the time since my last insulin dose. A Timesulin timer replaces the lid of a normal insulin pen and has a clock on it, which starts its timer every time the lid is clicked back onto the pen. That way it measures the time between injections. I sometimes forget to inject at lunchtime, when I am running around, and so find this really useful when I can’t remember whether I have given myself a meal-time injection.
The needles used to be 12mm long but most people now use 4mm needles, which are a lot more comfortable.
Many people with type 1 now use insulin pumps to help improve their blood glucose targets. Many blood glucose meters now provide detailed read-outs and will also give you a reading no matter how low your blood glucose goes. If pricking your fingers makes your fingertips sore, you can probably find a softer finger-pricker and several of these have adjustable depths.
Different ketone test strips will check for ketones in your blood or urine, although it is recommended to check blood ketones if you have type 1 diabetes.
People with type 1 diabetes are advised to check for blood ketones if they feel unwell, even if blood glucose is not high. Some blood glucose meters will test for both blood glucose and blood ketones but using separate strips. Checking for blood ketones should be part of everyone’s sick day rules, which is important information about what to do when you are ill.
Flash Glucose monitors
The biggest life changer for me, after doing the Dose Adjustment for Normal Eating Course (DAFNE) course, was when I started self-funding the Freestyle Libre flash glucose monitoring (FGM) system a couple of years ago.
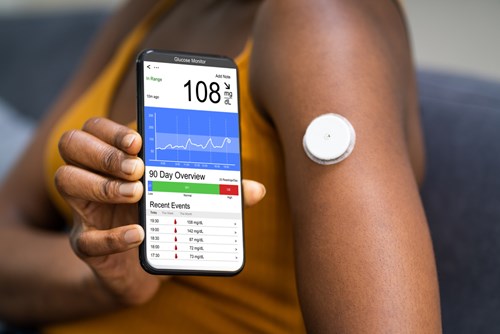
Now I have continuous blood glucose monitoring 24 hours a day for 14 days at a time (this is how long each sensor lasts), with readings every 5 minutes recorded graphically on a reader (or a smartphone app) together with my latest reading. The reading on the Libre lags behind the normal finger prick number by 10 minutes.
There are also really helpful arrows indicating whether my blood glucose is going up or down and the speed of the rise or fall.
If you use the smartphone to scan your Freestyle Libre sensor, then the results can quickly be shared with your healthcare team, if you want to.
For the first time, I was able to see that my blood glucose was dropping while I was asleep, often for quite long periods.
Continuous glucose monitors
However, I felt that I needed an alarm to wake me up when my blood glucose dropped low overnight as this can be risky. Enter the alarmed Dexcom G6 continuous glucose monitor (CGM).
Because of the risk of hypos in the elderly (I am 76) causing abnormal heart rhythms and serious complication, such as stroke and heart attack, combined with my lack of night-time hypo awareness, I am now using an NHS funded CGM and I am having far fewer episodes of low blood glucose often because of the advanced notice provided by the alarm.
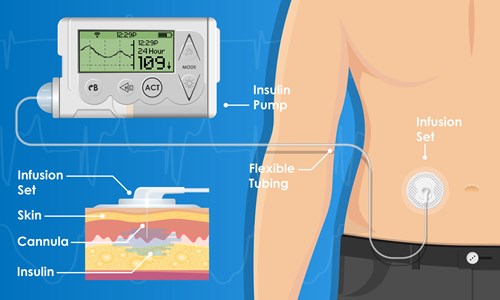
Insulin pumps, otherwise known as continuous subcutaneous insulin infusion (CSII) therapy have been around for over 35 years now. They are getting smarter and smarter and several can vary both your background insulin and your mealtime bolus requirements at different times of the day.
They can be titrated minutely to deal with things like exercising, travelling and pregnancy. The cannula usually needs replacing every three days. The Omnipod pump system connection to the controller is tubeless whilst already the Medtronic Minimed Paradigm Veo system will provide a link between its insulin pump and a glucose sensor, with an automatic insulin shut-off mechanism when one’s BG falls to a pre-set level.
What’s next?
The next development, a closed loop system that works like an artificial pancreas to automatically dispense the correct amount of insulin for one’s BG readings as they change throughout the day, is at this time only available on an unregulated ‘Do It Yourself' basis.
We may have to wait a while for a commercial version, but what a distance we have come from that glass syringe and a single type of insulin.




